If you’re living with a kidney transplant, you know the stakes are high. Your survival depends on keeping your immune system in check without harming the graft. Two heavy hitters do this job: tacrolimus and cyclosporine. Both belong to a class called calcineurin inhibitors. They are the backbone of post-transplant care, preventing acute rejection. But here is the hard truth we often ignore: generic versions of these life-saving drugs can cause major blood level fluctuations. While saving money sounds great, a drop in drug levels means a higher risk of rejection. Many doctors prefer brand names because the consistency matters more than the price tag when your organ is at stake.
Understanding the Core Medications
To understand the problem, we must look at the drugs themselves. Cyclosporine was the pioneer, approved by the FDA in 1983. It blocks calcineurin phosphatase activity by binding to cyclophilin proteins. This stops T-cells from activating and attacking your new organ. Tacrolimus, approved in 1994, does something similar but binds to FK-binding proteins instead. Despite different binding partners, both suppress interleukin-2 transcription. This similarity is why people assume generic substitutions should be safe. However, the sensitivity varies wildly between individuals.
| Attribute | Tacrolimus | Cyclosporine |
|---|---|---|
| Molecular Weight | 804 g/mol | 1203 g/mol |
| Daily Dose Example | 5 mg twice daily | 150 mg twice daily |
| Therapeutic Range (ng/ml) | 5-15 ng/ml | 100-200 ng/ml |
| Typical Monthly Cost (Generic) | $300-$500 | $150-$300 |
Note the molecular weight difference. Tacrolimus is significantly lighter, which contributes to better tissue penetration and lower required concentrations. Because of this potency, even small manufacturing variances in a generic tablet matter more for tacrolimus than for many other drugs. We see dosing reflected in the numbers above; a tiny change in absorption translates to a large percentage change in blood concentration.
The Generic Substitution Dilemma
Insurance companies love generics. In the United States, Medicare Part D formulary requirements drive adoption. As of 2023, over 92% of patients receive generic versions. There is a logic here: branded Prograf can cost $1,500 monthly while generic versions sit around $500. For families paying out of pocket, that is a huge difference. However, the medical community worries about "interchangeability." Different manufacturers use different fillers, binders, and coating technologies.
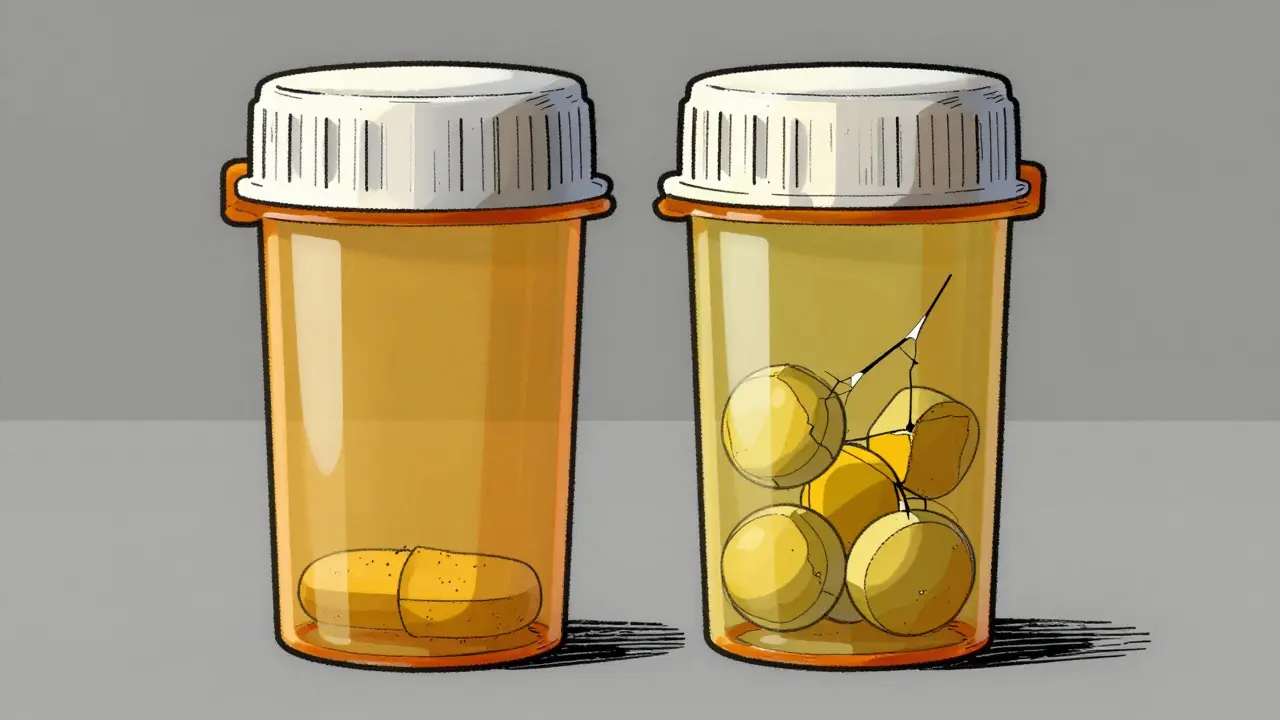
Consider the experience of a Reddit user named KidneyWarrior. After switching from brand Prograf to a generic, their levels plummeted from 8.5 to 5.2 ng/ml in two weeks. This wasn't just a number on a page; it led to a hospital admission for a mild rejection episode. This story highlights the reality of the narrow therapeutic index. If you are on tacrolimus, your acceptable range is tight-often just 3 to 15 ng/ml. A standard deviation of 20% in generic formulation can push you outside that window.
Manufacturers claim bioequivalence studies prove safety. The FDA requires confidence intervals within 80-125% for area under the curve (AUC) and peak concentration (Cmax). Yet, these studies often use healthy volunteers rather than transplant recipients. A patient’s metabolism changes with time, diet, and infection status. What works for a healthy volunteer might fail someone recovering from surgery. The European Medicines Agency recognized this gap. In February 2024, they issued updated guidelines demanding bioequivalence studies using actual transplant patient populations.
Clinical Evidence and Outcomes
Data supports the concerns. Research from 2005 by Dr. BK Krämer showed significant benefits for tacrolimus over cyclosporine regarding acute rejection. Biopsy-proven rejection occurred in 19.6% of tacrolimus patients versus 37.3% for cyclosporine. The renal function numbers were also better long-term. Serum creatinine levels remained lower in the tacrolimus group at two years. Despite this, patients face specific side effect risks. Tacrolimus increases the chance of post-transplant diabetes mellitus (PTDM) significantly-roughly 20% compared to 4% for cyclosporine.
When switching brands or moving to generics, instability becomes the main enemy. A 2022 survey by the American Society of Transplantation found that nearly 43% of recipients reported side effect changes after switching to generic tacrolimus. Over 18% needed dose adjustments to manage unstable levels. This isn't just theory. Real-world adherence drops by about 15% when patients perceive the medication isn’t working. Fear drives behavior. If levels fluctuate, patients get anxious. Anxiety leads to skipping doses or taking them inconsistently, creating a cycle of failure.
Graft survival is another metric. Studies show long-term graft survival rates are similar between the two drugs, but the path gets messy with generics. The composite endpoint of graft loss, patient death, or acute rejection occurred much more frequently in cyclosporine arms of older studies. Today, most centers default to tacrolimus because it wins on efficacy. However, the "generic trap" undermines those wins. A patient getting the best drug but receiving inconsistent dosing loses the benefit.
Managing Risk and Protocols
You cannot simply buy the cheapest bottle and stop worrying. Pharmacist protocols matter. The American College of Clinical Pharmacy recommends weekly monitoring for the first month after any switch. In practice, many centers require four to six weeks of intensified monitoring. This isn't always done. Community resources exist, like the National Transplant Insurance Assistance Fund, which helped thousands navigate forced switches in 2023 alone.
How do you stay safe? First, stick to one manufacturer. Some transplant programs now negotiate contracts with a single generic supplier to minimize switching variables. Second, watch the timing. Take your medication within a strict one-hour window every day. Third, avoid interactions like grapefruit juice, which messes with CYP3A4 metabolism and spiking your levels unpredictably. If you notice tremors or numbness in fingers, report it immediately. These are signs your level has spiked too high. Conversely, fatigue and fever might signal levels dropping low.
| Sign | Possible Cause | Action Required |
|---|---|---|
| Tremor/Paresthesia | High Blood Levels | Contact doctor, hold dose if instructed |
| Fever/Fatigue | Low Blood Levels | Urgent lab draw required |
| Diarrhea/Gum Swelling | Formulation Change | Monitor levels closely |

Future Developments and Genetic Testing
We are seeing movement toward smarter dosing. Pharmacogenetic testing allows doctors to look at your CYP3A5 genotype. Knowing your genetics cuts the time to reach therapeutic levels by roughly 63%. Companies like Astellas Pharma are also developing extended-release formulations. An LCP-tacrolimus version received approval in late 2023. The goal is flattening the peaks and troughs in blood concentration, theoretically making switching safer. While promising, widespread adoption takes time. Most patients still rely on immediate-release tablets.
Long-term market analysis predicts generic dominance through 2030. Experts project that over 95% of prescriptions will be generic by then. This shift forces clinicians to adapt. We need to move away from blind trust in substitution. The International Transplant Society emphasized in 2024 that individualized management is mandatory. You shouldn’t treat everyone the same. Your metabolism determines your tolerance.
Frequently Asked Questions
Is generic tacrolimus safe?
It is FDA-approved as bioequivalent, but real-world data shows frequent level fluctuations. Safety depends on strict monitoring during and after a switch.
Why do some doctors refuse generic substitutes?
Doctors avoid generics due to narrow therapeutic windows. A minor variance in absorption can lead to rejection or toxicity, outweighing cost savings.
How do I prepare for a medication switch?
Get a baseline blood test before switching. Monitor levels weekly for at least one month afterward. Keep a log of symptoms like tremors or energy levels.
What is the cost difference between brand and generic?
Branded tacrolimus costs roughly $1,200 to $1,500 per month. Generic versions typically range from $300 to $500. Cyclosporine sees similar savings.
Can I take different generics on different days?
No. Different batches or pharmacies may source from different manufacturers. Always request the same specific manufacturer to maintain stable blood levels.






Victor Ortiz
April 1, 2026 AT 15:18The statistics regarding bioequivalence margins are often misinterpreted by the general public during these discussions. Manufacturers claim safety within narrow windows while ignoring individual metabolic variances entirely. We see data suggesting rejection rates spike significantly when switching between specific generic formulations repeatedly. Insurance providers prioritize cost reduction metrics over graft survival rates in their decision-making processes. It is unfortunate that patient advocacy groups do not have stronger leverage against these corporate policies. The FDA guidelines remain insufficient for protecting vulnerable transplant populations adequately. We need stricter mandates on reporting adverse events linked to formulation changes specifically. Generic substitution creates a statistical probability problem that doctors simply cannot manage alone. Patients bear the brunt of systemic failures within the pharmaceutical supply chain currently. Real world evidence proves that consistency in medication matters far more than price tags suggest. Financial savings are meaningless if the organ is rejected due to absorption variance issues. Healthcare systems must treat these immunosuppressants differently than standard antibiotics or painkillers.
Amber Armstrong
April 1, 2026 AT 20:03I hear how hard this situation is for everyone navigating these complex medical decisions daily. Your experience with level fluctuations resonates deeply with many in our community support groups locally.
It feels like you are constantly walking a tightrope with your health hanging in the balance always. Trusting the pharmacist becomes difficult when you know different batches might behave differently inside your body. We spend so much time tracking symptoms instead of enjoying moments of normalcy in life. The fear of rejection shadows every meal and every interaction with new medications prescribed. Friends sometimes do not understand why we obsess over the specific pill bottle labels provided. They think a generic drug is chemically identical to the brand version in every way possible.
That assumption causes a lot of unnecessary stress for families trying to manage limited financial resources. Monitoring blood work weekly adds another layer of anxiety to an already overwhelming schedule quickly. Small changes in how we feel physically can signal big problems under the surface layers. It takes immense courage to advocate for yourself with aggressive medical professionals firmly. You deserve better stability from the healthcare institutions designed to help us survive surgery. Please remember that your vigilance is what keeps your graft functioning properly today.
Communication gaps between specialists often lead to confusion about which supplier produced the latest stock. Consistency in timing also plays a massive role alongside the manufacturer identity issue specifically. Hope remains a powerful tool even when the road ahead looks incredibly steep and dangerous. Your journey inspires patience in those watching your progress from afar closely. Keep fighting for the stable dosages that your body absolutely needs right now. We are here listening to every word you share about your struggle today.
Calvin H
April 1, 2026 AT 22:08Insurance companies clearly care more about their quarterly earnings reports than human lives.
Dan Stoof
April 3, 2026 AT 18:38This information IS exactly what we need to fight back against the system!!! It feels empowering to know that small changes matter SO MUCH for our safety!!! We can win this battle by demanding strict adherence to brand names consistently!!! Do not let anyone tell you that generics are always perfectly interchangeable safely!!! Your health is worth the extra investment in peace of mind definitely!!! We have seen miracles happen when patients stick to one source diligently!!! Stay strong and never give up on finding the perfect regimen soon!!! Knowledge is power and armed with this truth you will thrive forward!!! Keep your levels stable and your spirit high through it all always!!! Victory is possible even when the odds seem stacked heavily against you now!!!
Carolyn Kask
April 5, 2026 AT 15:13Foreign regulations lag behind American standards when it comes to approving these critical medications effectively. We should rely on domestic testing data rather than international oversight records specifically. It is ridiculous that European agencies get involved before we fix our own pipeline gaps. Americans want safety above foreign influence in their own healthcare infrastructure entirely. The FDA should mandate stricter transparency on manufacturing variances before allowing distribution widely. We lose trust in the system when politicians ignore these medical nuances completely. Taxpayers fund research but patients get stuck with cheap alternatives unexpectedly. National security includes public health security during these global supply chain crises. Stop importing uncertainty into American treatment plans for sensitive conditions immediately. We deserve the best protection available within our borders fully.
Katie Riston
April 7, 2026 AT 01:37The intersection of ethics and economics creates a complex moral landscape for all stakeholders involved. We wonder if profit motives inherently conflict with patient survival goals fundamentally. Life extension technologies should perhaps prioritize access over maximum revenue generation. Philosophers argue that bodily autonomy includes control over chemical intake sources directly. When society dictates medication brands via insurance formularies it diminishes personal agency significantly. We must consider the dignity of the recipient during these high-stakes negotiations. Cost cutting measures often overlook the intangible value of stability in recovery timelines. Ethical frameworks must evolve to address pharmaceutical inconsistencies more robustly. True justice means aligning financial incentives with health outcomes transparently. The balance shifts when we view patients as partners rather than expenses.
Brian Yap
April 7, 2026 AT 14:39G'day mates, just wanted to drop in from Down Under regarding these issues. Over here in Oz we face similar struggles with pharmacy scripts changing constantly. It is bloody frustrating trying to maintain consistent levels with shifting suppliers. Kiwi and Aussie transplant communities chat about this nightmare often. We just want the doctor to sign off on one batch code. Staying vigilant helps us stay alive for longer periods comfortably. Cheers for sharing the detailed breakdowns on the chemistry specifics. Keep your heads up and look after your grafts well. Plenty of us are dealing with this mess globally. 👋
Ruth Wambui
April 7, 2026 AT 19:05There are shadowy forces controlling which pills reach our medicine cabinets secretly. Big Pharma orchestrates these shortages to force compliance with their proprietary formulas. They know our metabolism better than we know ourselves intimately. Genetic testing allows them to predict our vulnerabilities before we speak. The extended release versions are merely steps toward deeper surveillance methods. We must read the ingredients lists like secret codes hidden in plain sight. Corporate greed drives these switches while whisper campaigns dismiss patient concerns. Beware of the glowing badges of official approval on misleading paperwork files. Truth lies in the blood work spikes that defy standard explanations. Wake up to the pattern of controlled chaos in our medical system today.
Marwood Construction
April 9, 2026 AT 13:38Current protocols indicate that therapeutic monitoring requires enhanced frequency during transitions. Clinical guidelines from the American Society of Transplantation highlight specific risk factors. Standard deviations in bioavailability necessitate rigorous oversight by licensed practitioners. Documentation of adverse events following substitution supports ongoing regulatory review processes. Stakeholders must recognize the correlation between formulation changes and rejection episodes. Compliance with strict dosing schedules remains the primary mitigation strategy available. Interdisciplinary teams should coordinate care plans to minimize disruption risks effectively. Longitudinal data collection improves future decision-making regarding brand selection. Evidence-based practice dictates that patient safety supersedes cost containment measures. Rigorous adherence to established medical literature prevents preventable complications universally.
William Rhodes
April 9, 2026 AT 21:36You outline the facts but we must conquer the obstacles standing in our way. Positivity drives physiological recovery in ways that doubt does not achieve. Fighting the generic trap starts with believing in your ability to manage it. We refuse to accept failure as an inevitable outcome of the current situation. Your discipline in monitoring levels builds a fortress around your health daily. Optimism is not blind hope but a strategic weapon against despair. Doctors respond better to confident advocates than passive recipients of care. Demand the best because you are worthy of the best treatment options. Never let bureaucracy dictate the limits of your potential survival. Stand tall and fight for the stability that keeps your organ working perfectly.